A one-time dose of an experimental stem cell treatment can repair brain damage and improve memory function in situations that imitate human strokes and dementia, a new study finds.
Dementia can arise from several situations, and it is considered by a range of symptoms including difficulties with memory, consideration, communiqué, and physical coordination. The two most common reasons for dementia are Alzheimer’s illness and white matter strokes – small strokes that accrue in the involving parts of the brain.
It’s a malicious cycle: The two main reasons for dementia are nearly always seen together and each one hastens the other.
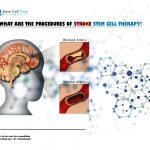
Presently, there are no treatments accomplished of stopping the development of white matter strokes or increasing the brain’s imperfect ability to repair itself after they happen. The new study recognizes a cell therapy can stop the progressive harm triggered by the illness and arouse the brain’s own repair procedures. The cells used in the treatment are a particular type of cells that surround and provision neurons in the central nervous scheme.
Upon injection, the cell therapy trekked to injured areas of the brain and concealed chemicals called development factors that enthused the brain’s stem cells to present a repair response. Actuating that the reparation procedure not only limited the development of harm but also improved the development of new neural contacts and amplified the creation of myelin – a fatty element that asylums and guards the connections.
Understanding the character that cell therapy play in revamping white matter harm is a critically imperative area of research that desires to be discovered. These initial results recommend that cell-based treatments may one day benefit battle the white matter damage that several strokes and vascular dementia patients ache every year.
That would set the therapy apart from patient-specific cell treatments, which are formed using each discrete patient’s own cells. While patient-specific cell treatments are pleasing because they do not need patients to take medicines to avert their immune systems from refusing the transplanted cells, they are also exclusive and can take weeks or months to crop.
The harm from white matter strokes is progressive, so you don’t have months to devote to making treatment for each patient. If you can have a therapy that’s already in the freezer prepared to go during the window of time when it could be most operative, that’s a much better choice.”
The brain is a predominantly good target for off-the-shelf cell treatments as the immune movement in the brain is extremely controlled. That feature, recognized as an immune privilege, lets donor cells or muscles that would be disallowed by other portions of the body endure for prolonged, even unspecified, stages.
Stem cell treatment procedure is exactly determined according to the patient’s illness and a dissimilar protocol may be applied for each patient. The most understandable and lasting effects of the therapy were gotten in the initial step of the disease, in which neurological and mental signs have seemed (in 90% of the cases). Positive consequences were also attained in patients with organic brain grazes (atrophy of the frontoparietal lobes).
As a result of the submission of stem cells in patients with significant illness, the excellence of life of the patients suggestively improved (general disorder, sleep, appetite, etc.) as well.