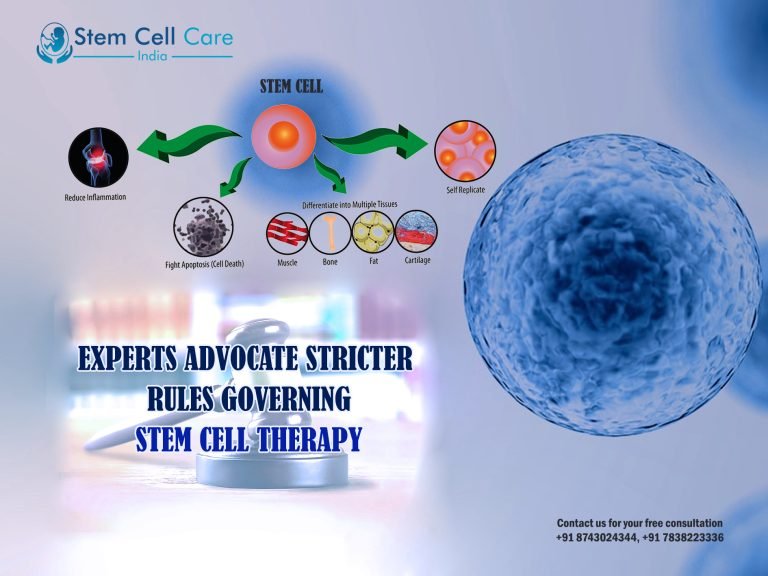
The Emerging Role of Amniotic Membrane Placental Cells in Regenerative Medicine

Amniotic membrane placental cells are cells derived from the amniotic membrane – an integral part of the placenta – that can have numerous properties. They include epithelial cells, mesenchymal cells and immune cells, and are known for their potential to help promote wound healing, reduce inflammation and modulate the immune response. Because of these properties, amniotic membrane placental cells have been used in certain medical applications, with individuals sometimes opting to receive amniotic membrane grafts to treat certain conditions.
The benefits of stem cells have been established by multiple clinical studies, prompting researchers to shift away from using embryonic stem cells. Recent discoveries showed that umbilical cord blood is full of stem cells, and that the placenta, otherwise discarded post-delivery, contains a greater abundance of stem cells when compared to cord blood. This finding also revealed that placental cells possess moderate surface antigens, allowing for usage with multiple patients. Similar to cord blood, placental cells can be banked and are highly manipulable multi-potent adult cells, ideal for therapeutic use.
Typically, placental stem cells are sourced from conventional childbirth or from mothers who opt to take the elective route of a Caesarean section. Stem cells derived from placenta have the same properties as those sourced from umbilical cord blood (UCB) and bone marrow. These multipotent cells have the potential to effectively treat chronic conditions such as leukemia, sickle cell anemia and thalassemia and in some ways, can be considered a natural pharmacy.
What are the Conditions That Can be Treated by Amniotic Membrane Placental cells?
 Investigation is ongoing to explore the full therapeutic applications of amniotic membrane placental cells due to their unique properties, including anti-inflammatory, wound healing, and immunomodulatory effects. To date, these cells have been studied in relation to treatments for a variety of diseases and conditions, such as:
Investigation is ongoing to explore the full therapeutic applications of amniotic membrane placental cells due to their unique properties, including anti-inflammatory, wound healing, and immunomodulatory effects. To date, these cells have been studied in relation to treatments for a variety of diseases and conditions, such as:
- Eye Disorders: The amniotic membrane, derived from placental cells, has become highly valuable in ophthalmology for its capacity to foster tissue repair, decrease inflammation, and safeguard the eye’s surface. This ability has been employed in the treatment of various ocular surface disorders, including corneal ulcers, chemical burns, and other types of eye injuries.
- Wound Healing: The regeneration-promoting properties and growth factors of amniotic membrane have been utilized to aid wound healing in many cases, such as chronic ulcers, diabetic foot ulcers, and surgical wounds. It can boost up the wound closure rate and accelerate healing.
- Orthopedic Applications: Studies on the use of amniotic membrane placental cells for orthopedic conditions such as osteoarthritis and tendon injuries have been conducted. These cells possess the ability to facilitate tissue regeneration and regulate inflammation, which could potentially be applied to support joint and tendon restoration.
- Cardiovascular Conditions: Studies have indicated that cells from the amniotic membrane and placenta may be able to aid the healing process after a heart attack or other cardiac injury, potentially facilitating heart tissue regeneration.
- Neurological Disorders: Research into the use of amniotic membrane placental cells to treat neurological disorders such as Parkinson’s disease and spinal cord injuries is in its early stages. However, due to their regenerative potential, these cells could be useful for repairing damaged nerve tissue and offer a promising treatment for these conditions.
- Inflammatory Diseases: Research has examined the use of amniotic membrane placental cells to treat symptoms associated with inflammatory conditions such as inflammatory bowel disease (IBD) and rheumatoid arthritis, due to the anti-inflammatory effects of these cells.
So far, over 180 severe blood disorders have been treated through stem cell transplants obtained from the umbilical cord and placenta, the majority of them from sibling donors.
Some additional diseases that are treated utilizing human- derived placental stem cells
- Autoimmune disorders such as multiple sclerosis, Crohn’s disease, and rheumatoid arthritis. Their immunomodulatory effects can help regulate the immune response and suppress inflammation.
- These cells have potential to slow down the progression of type 1 diabetes by modulating the immune response and protecting insulin-producing cells.
- Placental stem cells have been explored for their wound-healing and skin-regenerating properties, making them potential candidates for treating conditions like chronic ulcers and burns.
- Conditions like chronic obstructive pulmonary disease (COPD) and idiopathic pulmonary fibrosis have been investigated for placental stem cell therapy due to the cells’ ability to reduce inflammation and promote lung tissue repair.
- Liver disorders, including liver fibrosis and cirrhosis, have been explored as potential targets for placental stem cell therapy.
The Process of Harvesting and Transplantation of Placenta-Derived Stem Cells
 Obtaining placenta-derived stem cells involves harvesting the placental tissue, processing the stem cells within it, and then transplanting them to the intended recipient. This procedure is done to provide therapeutic benefits. Here is an outline of the general protocol involved in this process:
Obtaining placenta-derived stem cells involves harvesting the placental tissue, processing the stem cells within it, and then transplanting them to the intended recipient. This procedure is done to provide therapeutic benefits. Here is an outline of the general protocol involved in this process:
The Accumulation Process of Placental Stem Cells
- Collection: The placenta is typically collected after childbirth, either from the mother’s own delivery or from a donor placenta (with appropriate consent). It is important to collect the placenta as soon as possible after delivery to ensure the viability of the cells.
- Processing: Once collected, the placenta is transported to a laboratory or processing facility. The placenta is cleaned, and the desired sections or tissues (such as the umbilical cord or amniotic membrane) are carefully separated from the rest of the placenta.
- Cell Isolation: The placental tissue is then enzymatically or mechanically processed to release the desired type of stem cells, such as mesenchymal stem cells (MSCs). These cells are usually isolated from the umbilical cord’s Wharton’s jelly or other specific regions of the placental tissue.
- Cell Expansion: After isolation, the stem cells may undergo a period of cell culture to allow them to proliferate and expand in number. This step is important to obtain a sufficient number of cells for therapeutic use.
Transplantation Method
- Preparation: Before transplantation, the harvested stem cells are typically prepared for delivery. This might involve further purification, quality control testing, and possibly genetic modification or differentiation into specific cell types, depending on the intended application.
- Route of Administration: Placenta-derived stem cells can be transplanted using various routes, depending on the disease being treated and the desired effects. Common routes include intravenous (IV) infusion, intramuscular injection, intra-articular injection, and localized application to target tissues.
- Monitoring and Follow-Up: After transplantation, patients are closely monitored for any adverse reactions or side effects. Depending on the diseases and treatment goals, follow-up assessments are conducted to track the progress of the therapy and determine its effectiveness.
If you would like to find out more about placenta-derived adult stem cells, please don’t hesitate to get in touch with us immediately.